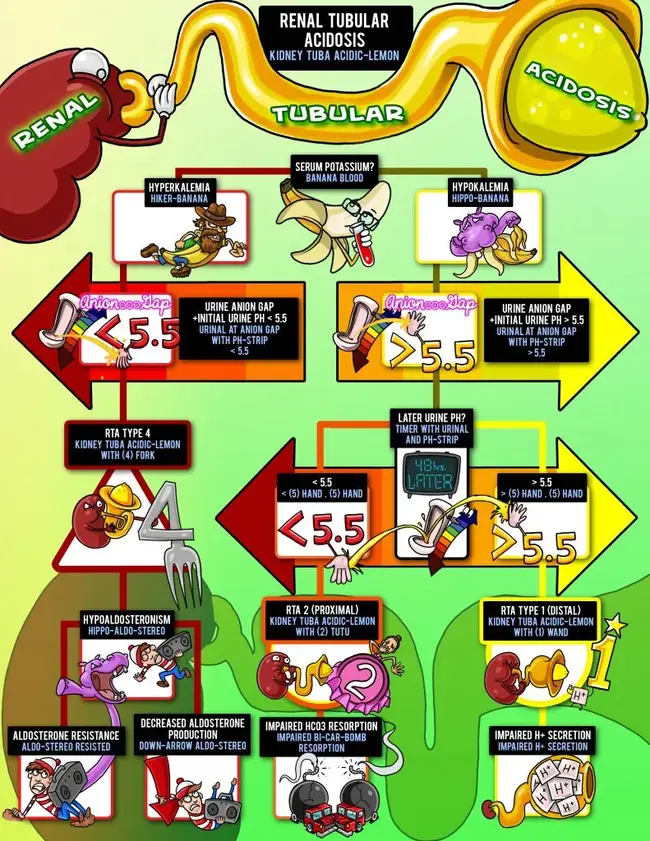
This visual algorithm will help you figure out how to diagnose and separate the different types of RTAs.
Some topics you will learn in this infographic:
Low Urine pH:
The hyperkalemia caused by the hypoaldosteronism impairs ammonia (NH3) genesis in the proximal tubule and therefore reduces the availability of ammonia to buffer urinary hydrogen ions. As there is an inadequate amount of NH3 available for buffering protons, the urine pH can decrease (<5.5).
Furosemide:
Furosemide is a loop diuretic that inhibits sodium and chloride resorption by competitively inhibiting the Na+/K+/2Cl- cotransporter in the ascending limb of the loop of Henle. It leads to potassium wasting. Therefore in some cases of hyperkalemic type 4 RTA, furosemide may be useful.
Familial Types:
Isolated proximal RTA can be due to inherited defects in genes involved in the synthesis of transmembrane transporters responsible for proximal acidification. The most common inherited defect is a mutation in the gene SLC4A4 that directs the synthesis of NBCe1, the basolateral sodium bicarbonate transporter. The inheritance pattern of this defect is autosomal recessive which means that to get the disease, the individual must have two copies of the defective gene.
Distal Tube:
The distal tubule is the segment of the nephron located between the ascending loop of Henle and the connecting tubule and collecting duct. Type I renal tubular acidosis is due to the inability of the intercalated cells of the distal tubule to secrete H+.
To learn more, get started with a free Picmonic account.